What Is Alcohol-related Pancreatitis?
Pancreatitis and alcohol are closely linked, as alcohol can cause pancreatitis, which is inflammation of the pancreas and should be considered as a warning sign that heavy alcohol use has progressed too far.
Something needs to be done immediately before more serious and tragic consequences occur. Drinking alcohol to excess is a principal cause of pancreatitis, which can have long-term consequences just as severe as cirrhosis and alcohol liver disease.
Pancreatitis is broken down into two separate forms.
First, there is acute alcoholic pancreatitis. Acute means that it will typically last just a short while and will clear up on its own or with some type of intervention. With pancreatitis, medical intervention is strongly recommended due to the severity of possible outcomes.
Acute pancreatitis can come from a variety of factors. It could be an infection, a cyst, or excess fluid buildup. An increase in alcohol consumption or long-term alcohol abuse can be the cause. The pancreas is a sensitive gland, and prolonged alcohol abuse can cause pancreatitis more rapidly than people often realise. (1)
The second type of pancreatitis is chronic alcoholic pancreatitis. Chronic means that it is a long-standing or lifelong disease that needs to be controlled or managed for a person to stay healthy and not feel its effects.
Chronic pancreatitis resulting from long-term alcohol use represents around seven out of 10 cases. You can expect this to happen after one or more bouts of acute alcohol-related pancreatitis. This is familiar territory, in other words. The damage, inflammation and scarring at this point will be too much for the body to heal, and it becomes a matter of trying to manage the symptoms.
If you drink alcohol in large amounts, you are advised to STOP. This can assist in the treatment of chronic pancreatitis.
Pancreatitis and Alcohol
Treatments for alcohol-induced pancreatitis will vary based on which type you have. While there is no cure for it, the body will often heal damage, or the symptoms will be treated and managed.
In acute alcohol-induced pancreatitis, the treatment will often consist of pain medication to manage its discomfort. Worst-case scenarios may include surgery to remove part of the scar tissue in the pancreas. The person with this disease may need to be monitored in a hospital setting to monitor their pancreatic functioning and overall well-being, such as an Ultrasound, CT scan, and MRI, which make images of your pancreas.
Chronic alcohol-related pancreatitis is most likely a lifelong illness to be managed at this point. However, what is known is that a person who quits drinking alcohol will typically stop the spread, and they may even be able to gain more functioning back in their pancreas.
The treatment is different for those with chronic alcohol-induced pancreatitis, although mainly focused on easing symptoms. Pain medication is still used for discomfort. There are more surgical options to help with removing scar tissue, improve insulin flow, unblock ducts, and relieve some of the pressure a person feels. Replacing pancreatic enzymes, taking insulin and following a strict diet is also part of the treatment protocols. Chronic alcohol-induced pancreatitis means that it will be with the person for their life and must be managed carefully.
Can Alcoholic Pancreatitis Be Cured?
The treatment for alcoholic pancreatitis is to quit drinking alcohol immediately. Stopping drinking alcohol can reduce or ease symptoms, or in the case of acute alcohol-related pancreatitis, clear it up quickly and help make it less painful. It increases life outcomes across the board, and with pancreatitis, no matter the type, it will reduce, remove, or ease symptoms. Individuals with alcohol-induced pancreatitis most likely have a moderate to severe alcohol use disorder. Remaining sober is a vital part of the treatment plan of anyone with alcoholic pancreatitis.
Participation in support groups, such as Alcoholics Anonymous or attending an alcohol treatment programme that includes an alcohol detox is recommended. Treatment at an alcohol rehabilitation centre will allow the individual to participate in intensive alcohol use group therapy and individual therapy to ensure continued alcohol abstinence.
What Is The Pancreas?
While it’s not as well known as the heart or the stomach, the pancreas plays a significant role in digestion and controlling how the body uses energy, including regulating blood sugar levels.
The pancreas is a gland located behind the stomach. It aids in the digestive process by secreting enzymes into the small intestine that help break down food that is in there. The small intestine does a great deal of digesting and breaking down food into absorbable nutrients.
One-third of people with chronic alcoholic pancreatitis have diabetes. This is because the damaged pancreas cannot make insulin for the bloodstream to control blood sugar levels. This is vital for overall health and dictates how the body uses and stores sugar for energy.
If a person develops alcoholic pancreatitis, the gland is damaged and inflamed. Becoming damaged and inflamed means that the enzymes secreted will not function properly and will be useless by the time they reach the small intestine. Instead, the digestive enzymes will try to break down the pancreas itself, as the body breaks down by attacking its own organs.
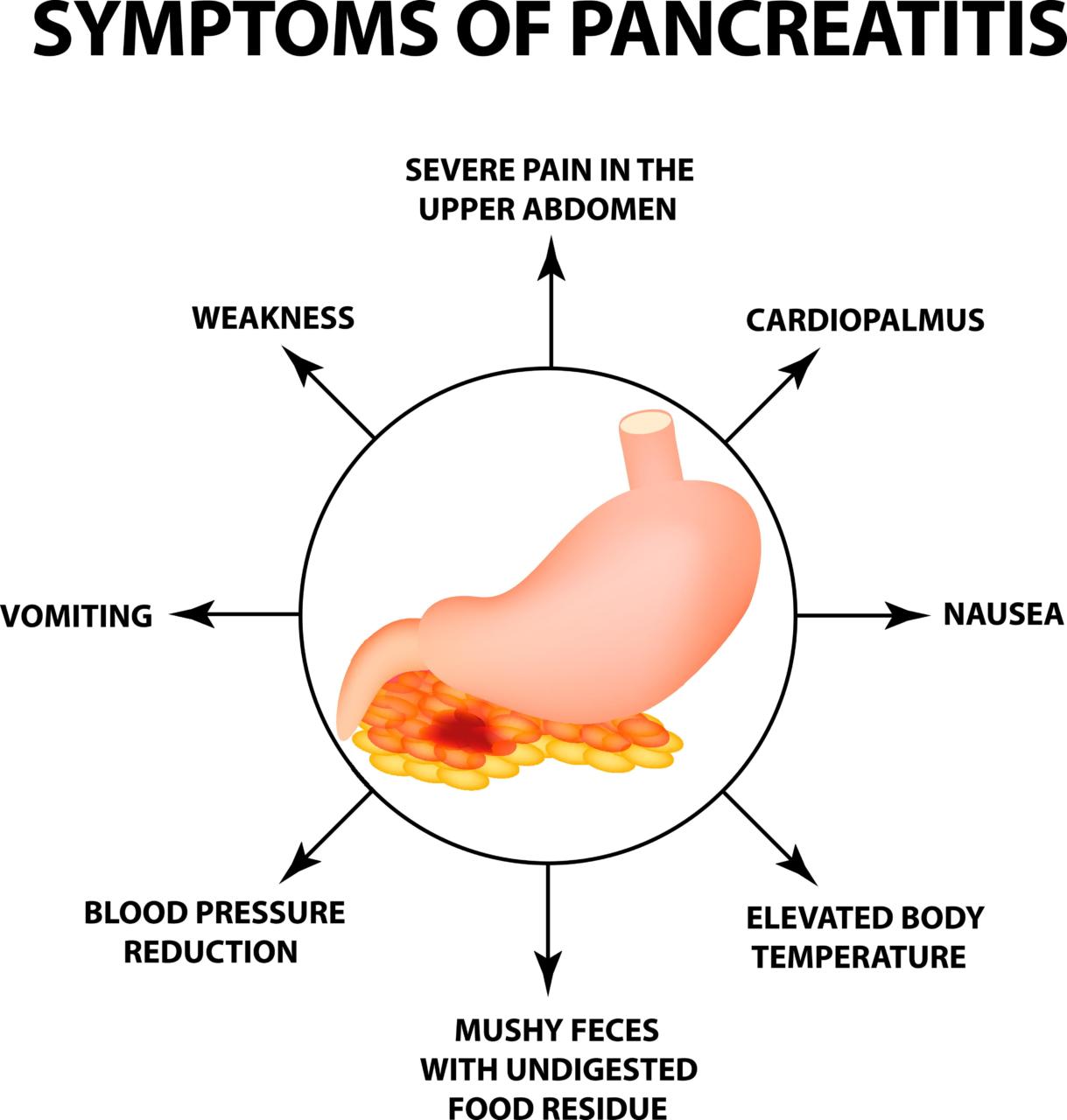
Alcoholic Pancreatitis Symptoms
- Abdominal pain. Pain will radiate and may be associated more closely with diet. Some foods like those high in fat cause more discomfort and pain.
- Feeling bloated
- Feeling tender or swollen in the belly
- Clammy skin
- Rapid heart rate
- Nausea/vomiting
- Low blood pressure
Diagnosing and treating the disease is very important. The sooner this is addressed, the sooner recovery can begin.
The Main Symptoms Of Chronic Alcoholic Pancreatitis
- Severe abdominal pain that can radiate and include back pain
- Unexplained weight loss
- Diarrhoea caused by poor absorption of food
- Diabetes due to damage making the pancreas unable to produce necessary insulin
- Jaundice
The Significant Causes of Pancreatitis
- Complications of surgery
- Hereditary issues
- High calcium levels in the blood
- Heavy alcohol use

Alcoholic Pancreatitis
Alcoholic pancreatitis may not always be the first thing someone thinks of when talking about pancreatitis, but it can have a lasting impact on their lives. The sad truth is that it does not have to be this way. Alcoholic pancreatitis can be managed or cleared up with sobriety. If you or someone you love is struggling with chronic health issues due to alcohol abuse, get help now. The sooner a person enters recovery, the better their health will become.
Our professional staff is looking forward to talking to you. Call us today at 0207 205 2845. You can also reach out to us by using our contact form. Our team will guide you on the best treatment options for your individual circumstances.
Sources
https://www.ncbi.nlm.nih.gov/books/NBK65575/
The National Pancreas Foundation
https://www.drinkaware.co.uk/facts/health-effects-of-alcohol/alcohol-related-diseases/alcohol-and-pancreatitis#:~:text=Chronic%3A%20You’re%20more%20likely,it’s%20worse%20if%20you%20smoke.
Jason has been writing expert articles and blog posts on issues related to addiction and mental health for Rehab Guide.
Jason has a BA in Psychology, a Masters of Social Work and is currently working on his doctorate in social work.


